Insights
TOP STORIES
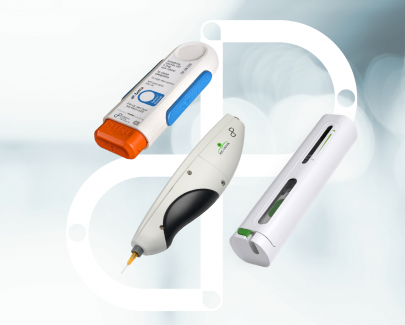
Whitepaper
Discover the future of parenteral drug delivery through expert interviews and real-world insights. Explore innovative strategies and design approaches driving improvements in usability, patient experience, and treatment outcomes.
Whitepaper
Discover the exciting possibilities on the horizon for inhalation device design. Explore recent advancements and innovative strategies crucial for developing significant new treatments.

Whitepaper
We’ve distilled the essence of successful diagnostic system development into this 10-minute guide – it’s your compass in the intricate world of diagnostics, highlighting critical considerations essential for turning ambitious ideas into tangible solutions.
OTHER INSIGHTS
CDP PRESENTS
THE INNOVATION STREAM
Short, insight-packed interviews exploring breakthrough developments in technology and design with experts at the top of their game.
WHITE PAPER
Breaking the mold: Digital tooling to reduce time to market
Getting new products to market efficiently is crucial to maximizing your return on investment.